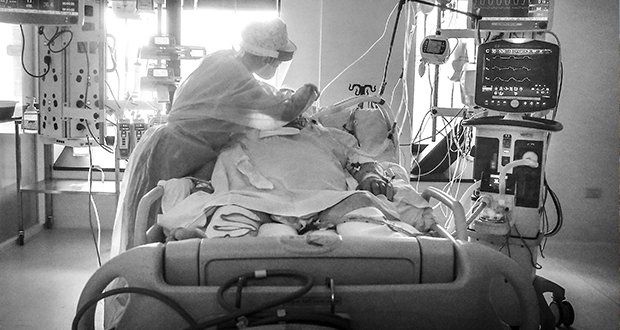
To date, many Australians who have died from COVID-19 have died alone and many others have missed out on visiting dying loved ones, but two Deakin University experts say it doesn’t have to be this way.
Writing for The Conversation, Associate Professor of Nursing Melissa Bloomer and Associate Head of School (International) Stephane Bouchoucha said there’s cause to consider whether Australia can do more to preserve the connection between patient and loved one at the end of life.
“There’s some variation between Victorian healthcare facilities in how visitor restrictions are applied,” the pair said. “Some allow visitors to enter hospitals for compassionate reasons, such as when a person is dying. But visitors are not permitted for patients with suspected or confirmed COVID-19.
“Family-centred care at the end of life in intensive care is a core feature of nursing care. So in the face of this unprecedented global pandemic, we realised we needed to navigate the rules and restrictions associated with infection prevention and control and find a way to allow families to say goodbye.”
Bloomer and Bouchoucha published a set of practice recommendations to guide critical care nurses in facilitating next-of-kin visits to patients dying from COVID-19 in ICUs.
The Australian College of Critical Care Nurses and the Australasian College for Infection Prevention and Control jointly endorsed the position statement.
The authors said: “The recommendations are evidence-based, reflecting current infection prevention and control directives, and provide step-by-step instructions for facilitating a family visit.”
Some of the key recommendations surrounded what visitors should do before coming to the hospital, how they can be guided through a visit and what they should be instructed to do when they return home.
Bloomer and Bouchoucha said: “It’s too early to know the full impact a loved one’s isolated death during COVID-19 may have on next-of-kin and extended family. But the effect is likely to be profound, extending beyond the immediate grief and complicating the bereavement process.
“These recommendations are not meant to be prescriptive, nor can they be applied in every circumstance or intensive care setting.
“We encourage intensive care teams to consider what will work for their unit and team.”
Click here to view the position statement.
Do you have an idea for a story?Email [email protected]
 Aged Care Insite Australia's number one aged care news source
Aged Care Insite Australia's number one aged care news source