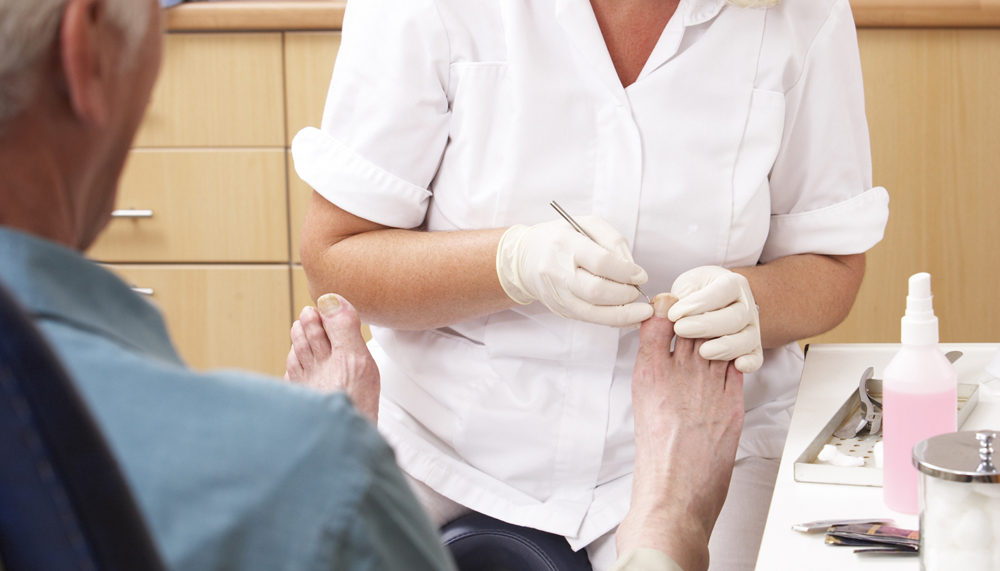
Podiatrists lobby for more national benefits to help detect and treat problems sooner.
The Australasian Podiatry Council wants the federal government to enable more Medicare-subsidised podiatrist visits a year, in line with National Health and Medical Research Council data stating that diabetes-related foot complications are becoming more prevalent in the elderly.
Confirming the council’s move, CEO Damian Mitsch says the podiatrists’ body is also asking for other reforms. “This is because of the positive impact their implementation would have on the health of the largest number of Australian patients, particularly those at high risk, and their ability to access subsidised regular consultations and services as needed,” the CEO says.
The council also wants podiatrist-enabled access to Pharmaceutical Benefits Scheme-subsidised testing, diagnostic imaging and podiatrist-enabled prescription services. “This means patients, especially with urgent conditions, would receive prompt treatment. [It would also help reduce duplicate appointments],” Mitsch says.
The federal government’s aged-care provider charter determines residential clinical needs, including health services such as podiatry. These include mandatory resident treatments by external specialists, including allied healthcare podiatry procedures – funded with assistance from Medicare – for diabetics or anyone with acute foot afflictions.
If the experience of Drummoyne-based podiatrist Lucasz Sempka is a guide, providing greater public access to podiatry means making it affordable to those in need. “In a lot of cases, feet may have been neglected for many years,” Sempka reports. He points to consumer spending choice as an understandable hindrance. “Someone with diabetes, for example, has spending choices, and podiatry costs money,” Sempka says. “Some people prioritise what they think they should spend, and don’t understand the consequences of making sure their feet are looked after.”
Mitsch goes further. “Standards in aged care around podiatric care are not well managed, because in the last 10 years we’ve seen a lack of focus on what was known as prescribed services, such as podiatry, and a poor understanding by standards assessors of what constitutes reasonable levels of allied health to maintain independence and activities of daily living,” he says. “This has been exacerbated by changes to aged-care funding tools over recent years, which have driven facilities to focus on documentation and dollars rather than the services prescribed as necessary for good care.”
Awareness of foot care in diabetics is highlighted in the Australian Diabetes Council’s public education campaigns. Its head of education and prevention, Kristen Hazelwood, says she has conducted regular talks and foot care screenings in registered clubs and community centres across NSW. She says foot afflictions such as peripheral neuropathy, or ulcers, are often neglected. This sometimes results from lack of awareness of an ailment because people don’t see the bottoms of their feet. “We teach people to look between their toes and for any irregular marks in the legs, or the skin on their feet, which should look as smooth as on their face,” Hazelwood says.
Podiatrists stress that more should be done for anyone with diabetes.
Some practitioners report that lack of awareness is an acute issue among clients. They say at-risk people, especially those with diabetes, often aren’t formally diagnosed. They also say Australia’s carer training methods warrant a closer look.
One podiatrist says infection happens all too often. Lower limbs are most at risk, especially among diabetics, as a result of poor pain response. “The practitioner needs to look at the bottom of a resident’s foot, because that is the diabetic person’s most vulnerable area,” the practitioner says.
European-trained pedorthist Paul Galy says that in a number of his cases in the past five years, lower limb amputations have been preventable. “The diabetic especially is at highest risk and sometimes a blood test, depending on time of day of the test aimed at revealing diabetes, does not show its presence,” Galy says. “And many diabetics are in denial.” Galy says the issue calls for more education of the carer and supervisor.
Senior clinical nurse adviser, diabetes, at the Royal District Nursing Service, (RDNS) Tracy Aylen, says foot care is an essential component of diabetes management to help prevent problems and identify any changes early. “A daily basic foot check is recommended as part of diabetes self-management,” Aylen says. “And a formal diabetes foot assessment should be attended at least yearly by a qualified health professional, such as a podiatrist.”
Aylen says assessments are attended more frequently if foot problems have been identified. Other health professionals – such as a GP, RN or diabetes educator – can attend a basic foot assessment and provide a referral to a podiatrist.
Aylen says many older people with diabetes use home care services, including personal care and this can help with prevention.
“As part of an individual’s healthcare team, the personal care worker has a role in reporting any adverse changes they may observe,” she explains. For example, a personal care worker undertaking duties such as helping a client shower would be expected to report any changes in skin integrity to their supervisor or the client’s nominated carer. However, personal care workers are not expected to undertake a foot assessment, Aylen says.
Part of Diabetes Australia’s (DA) strategy in 2013 includes developing and enacting national programs, with targets for primary care. Hospitals and diabetes centres would focus on prevention and complications by creating integrated multidisciplinary care and by measuring and reporting prevention of foot and limb complications and lower limb amputations. DA reports amputations as 15 times more common in people with diabetes – more than 20,000 diabetics have had lower limb amputations over the past decade.
Do you have an idea for a story?Email [email protected]
 Aged Care Insite Australia's number one aged care news source
Aged Care Insite Australia's number one aged care news source